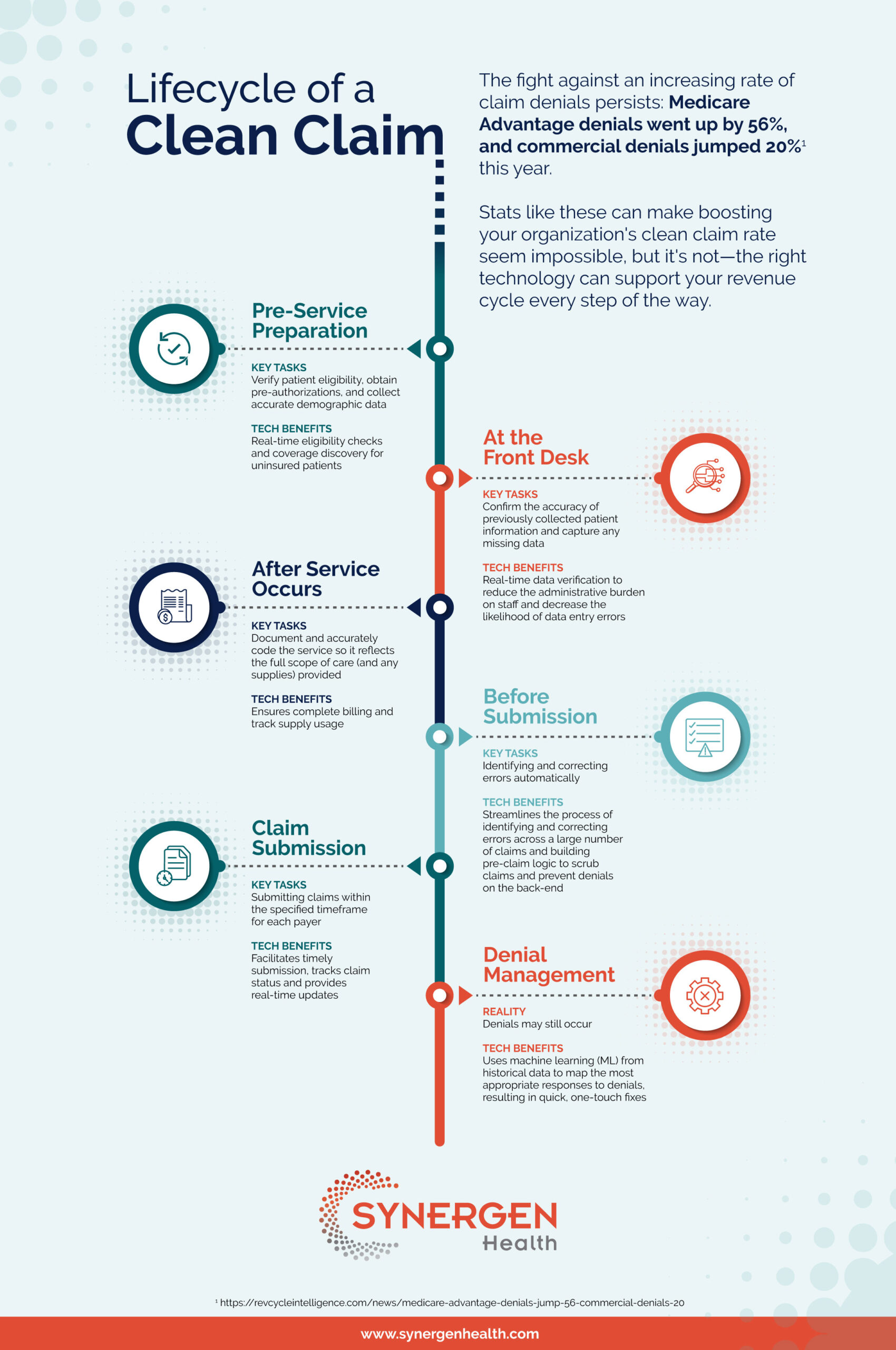
Lifecycle of a Clean Claim
The fight against an increasing rate of claim denials persists: Medicare Advantage denials went up by 56%, and commercial denials jumped 20% this year.
Stats like these can make boosting your organization’s clean claim rate seem impossible, but it’s not—the right technology can support your revenue cycle every step of the way.
Pre-Service Preparation
Key Tasks: Verify patient eligibility, obtain pre-authorizations, and collect accurate demographic data
Tech Benefits: Real-time eligibility checks and coverage discovery for uninsured patients
At the Front Desk
Key Tasks: Confirm the accuracy of previously collected patient information and capture any missing data
Tech Benefits: Real-time data verification to reduce the administrative burden on staff and decrease the likelihood of data entry errors
After Service Occurs
Key Tasks: Document and accurately code the service so it reflects the full scope of care (and any supplies) provided
Tech Benefits: Ensures complete billing and track supply usage
Before Submission
Key Tasks: Identifying and correcting errors automatically
Tech Benefits: Streamlines the process of identifying and correcting errors across a large number of claims and building pre-claim logic to scrub claims and prevent denials on the back-end
Claim Submission
Key Tasks: Submitting claims within the specified timeframe for each payer
Tech Benefits: Facilitates timely submission, tracks claim status and provides updates
Denial Management
Reality: Denials may still occur
Tech Benefits: Use machine learning (ML) from historical data to map the most appropriate
Responses to denials, resulting in quick, one-touch fixes
Promoting Clean Claims With the Right Technology
Want to dive deeper into how technology can help at every stage of the claim lifecycle? Check out our in-depth explanation.
If you’re curious about how end-to-end RCM services could help your organization, let’s chat.